1chap2_p_1This chapter provides the background and rationale for the User Guide. It explains why health is central to sustainable development, outlines the current financing challenges related to health systems in African countries and introduces the key financing instruments outlined in the resource. It also begins to identify everyday health expenditures and indicators that lend themselves well to these external financing options, as well as key considerations that governments must take into account when choosing the indicators.
Why Health Matters
2chap2_p_2Health is both a moral imperative and a foundation for economic and social development. The global community’s commitment to health is enshrined in the Sustainable Development Goals (SDGs), particularly SDG 2 (Zero Hunger) and SDG 3 (Good Health and Well-being). These set ambitious goals to substantially and sustainably improve the health of all people. Yet, beyond moral obligation, the case for investing in health is also profoundly economic. Healthier populations are more productive, more resilient and more capable of driving long-term national growth.
3chap2_p_3Evidence from across regions shows that investments in health yield among the highest returns of any public expenditure. Global analyses from the World Health Organisation (WHO) and the Global Fund suggest an average return on investment exceeding 30:1. These gains reflect the multiple channels through which health fuels development, from reducing absenteeism and increasing labour productivity to enhancing children’s learning outcomes and enabling women’s greater participation in the workforce.
4chap2_p_4Most importantly, health remains one of the issues citizens care about the most. The 2024 Afrobarometer survey found that health ranks second, on average, among the most critical problems for governments to address, behind only unemployment. This demand reflects a simple reality: when people are healthy, communities thrive, economies function and social contracts are strengthened.
5chap2_p_5For policymakers, therefore, investing in health is not just about meeting humanitarian goals; it is about safeguarding the very foundations of growth and stability. Recognising this link between health and prosperity is essential for both Ministries of Health (MoHs) and Ministries of Finance (MOFs) as they navigate the choices and trade-offs that shape national development.
The Funding Crisis
6chap2_p_6Over the past two decades, Africa has made remarkable gains in health: access to care has expanded, maternal and child mortality have fallen, and coverage of key services, such as immunisation, human immunodeficiency virus (HIV) treatment and other disease programmes, has increased significantly. These achievements reflect the dedication of governments, communities and development partners working to strengthen health systems and broaden service reach.
7chap2_p_7Much of this progress has been underpinned by external financing. For years, organisations such as the Global Fund, Gavi, the World Bank and significant bilateral donors have provided the resources that have helped to close domestic funding gaps.
8chap2_p_8That financial landscape is now changing rapidly. In 2024, total Official Development Assistance (ODA) from the Organisation for Economic Co-operation and Development - Development Assistance Committee members declined by 7.1% in real terms. In 2025, countries in sub-Saharan Africa are expected to see a 16-28% reduction compared to 2021, the most significant reduction among all regions. Additionally, health-specific aid is declining at a faster rate than other sectors. The most prominent donors, accounting for 80% of bilateral health and population aid, are expected to reduce their ODA contributions, with the United States alone providing over half of the historical contributions. These contractions occur at a time when health systems are under increasing pressure, as evidenced by the 41% increase in public health emergencies between 2022 and 2024.OECD. (n.d.). Official development assistance (ODA). Organisation for Economic Co-operation and Development. https://www.oecd.org/en/topics/policy-issues/official-development-assistance-oda.html
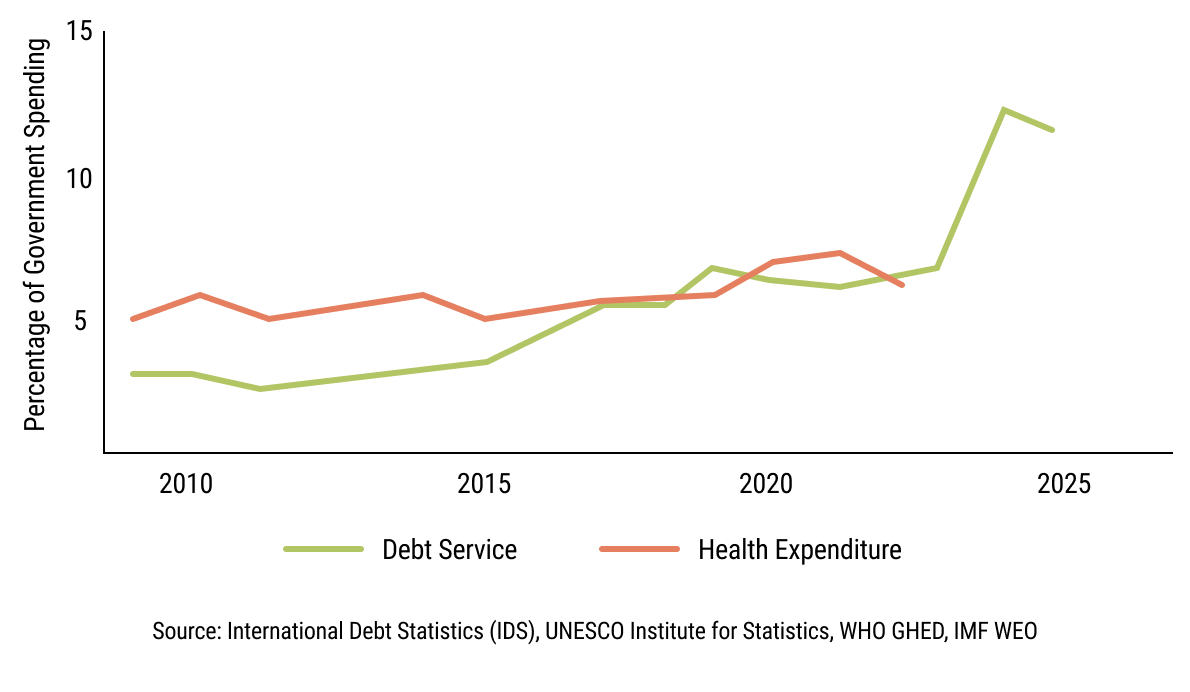
9chap2_p_9The decline in donor funding is exacerbated by a dramatically tightening fiscal space within African governments. At least 22 countries on the continent are now in or at high risk of debt distress, and more than 30 countries pay more annually on debt servicing (the total amount of money required to pay the interest and principal on existing debt) than on their health sectors.
 chap2_img_0
chap2_img_010chap2_p_10This triple pressure - shrinking external support, increasing healthcare needs and increasing debt servicing on existing debt obligations - forces governments to balance the imperative of improving health outcomes with the need to preserve macroeconomic fiscal stability. The result is a growing mismatch between what citizens need and what national budgets can sustainably deliver.
11chap2_p_11This is where collaboration between MoHs and MoFs becomes essential. Together, they must look beyond traditional budget allocations to identify and implement financing instruments, such as public-private partnerships (PPPs), debt swaps and other sustainable debt instruments that can expand fiscal space for health while maintaining financial sustainability. They should also consider the shifting roles of major health funders, such as the Global Fund, Gavi and the World Bank, as described in Chapter 4: Health Finance and Key Performance Indicators.
Case Study: Situating This User Guide Within National Health Financing Strategies12chap2_p_12Every country’s path to universal health coverage (UHC) is unique, but the principles of sound health financing remain the same. Health financing strategies are designed to chart a financially feasible pathway toward UHC, ensuring that everyone can access the health services they need without suffering financial hardship. Progress is measured along three dimensions: the range of services provided, the share of the population covered and the extent to which individuals are protected from out-of-pocket costs. 13chap2_p_13Within this broader framework, this User Guide offers practical options for governments seeking to increase health expenditure and move closer to UHC sustainably. It focuses on three financing instruments - PPPs, debt swaps and sustainable debt instruments - that can help countries mobilise and channel additional resources for health. However, these options are not stand-alone solutions. They should be considered complementary tools that operate within and are guided by a country’s overarching health financing strategy. 14chap2_p_14As the WHO Health Financing Guide explains, effective financing systems rely on three interconnected functions:
15chap2_p_15The instruments discussed in this User Guide primarily strengthen the first of these functions - resource mobilisation - while also linking to aspects of strategic purchasing, particularly through the PPP approach and impact bonds. 16chap2_p_16It is important to emphasise that this User Guide is not a substitute for a comprehensive health financing strategy. MoHs should continue to lead on developing and updating such strategies as a roadmap toward UHC - setting priorities, defining service packages and identifying reforms that improve efficiency and effectiveness. This includes maximising the impact of existing budgets through better prioritisation, stronger budget execution and more effective provider payment mechanisms. 17chap2_p_17Ultimately, the guidance provided here is intended to complement those broader efforts - equipping MoHs and MoFs with the tools, language and frameworks needed to explore new financing opportunities, while maintaining alignment with national health goals and fiscal sustainability. |
Proposed Solutions
Overview of Financing Structures
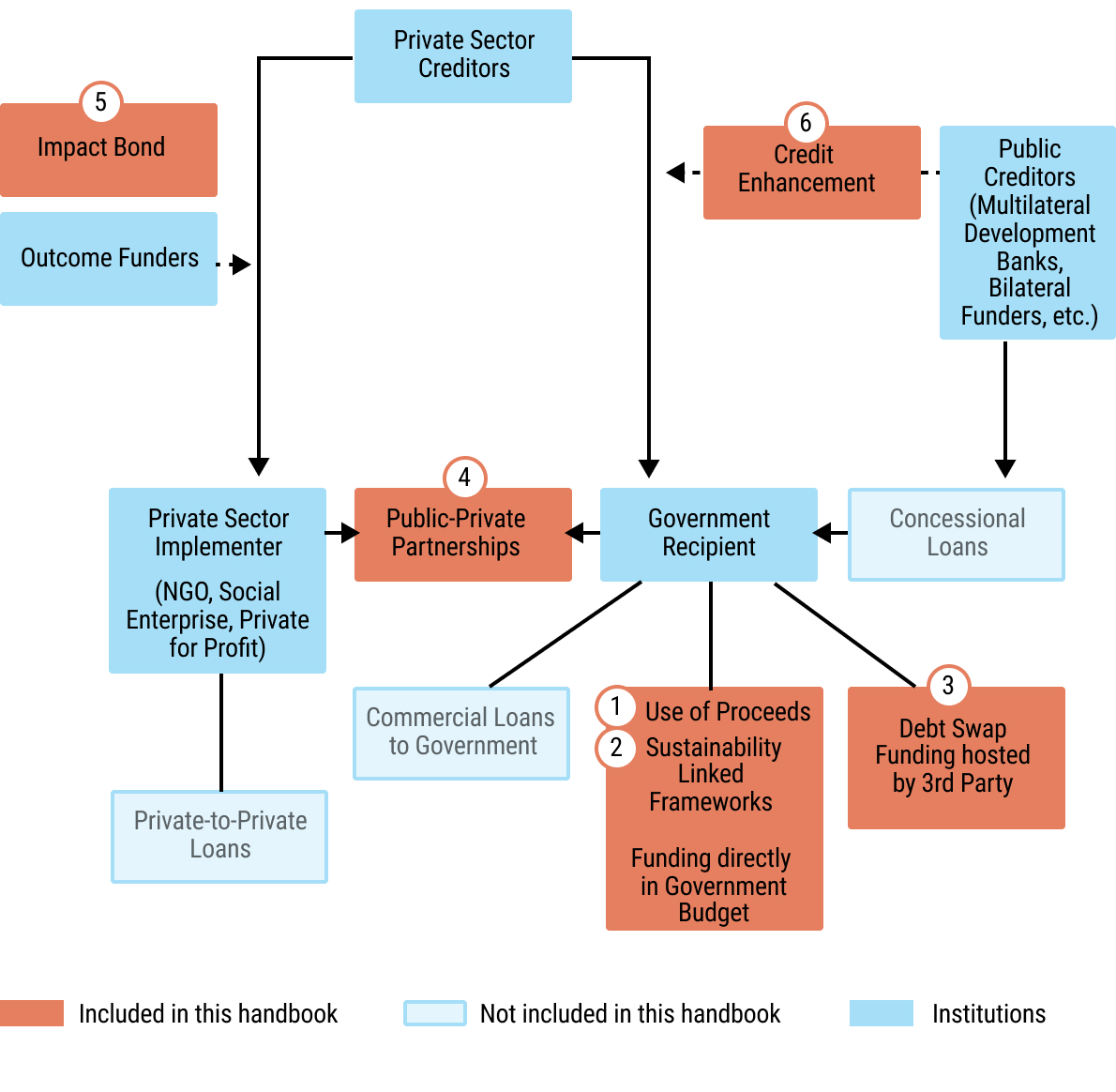
18chap2_p_18Several potential solutions exist for filling the financing gap that can be used simultaneously. This User Guide focuses on three categories of instruments, some of which have been rarely used in the health sector. However, they provide promising new opportunities for additional funding in the health sector. The User Guide does not address private funding that is channelled towards private sector implementers, but instead focuses on raising funds for the public sector. These instruments have been prioritised based on the African Legal Support Facility’s (ALSF) experience in responding to country requests for technical assistance in exploring and implementing them.
 chap2_img_1
chap2_img_1
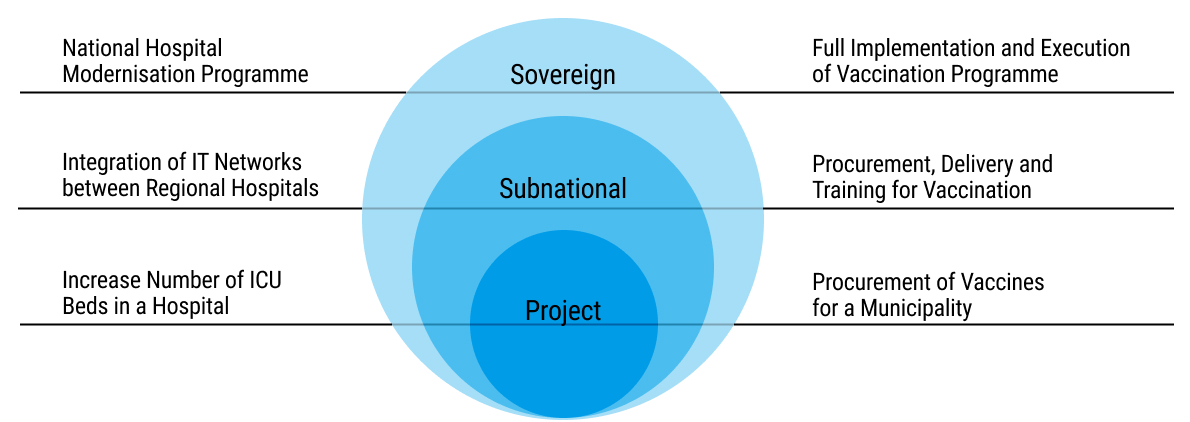
19chap2_p_19These instruments can be applied across different levels: the sovereign level (I.e. national level), sub-sovereign level (I.e. state or county level) or based on a specific project:
20chap2_p_20
 chap2_img_2
chap2_img_2
Financing Instruments
21chap2_p_21Some of the financing solutions discussed in this User Guide are novel to the health sector but have already been successfully used in other sectors. For instance, sustainable financing solutions often include those focused on deforestation or renewable energy, as well as debt swaps for marine conservation or education. PPPs, in contrast, have been in use in the health sector since the 1980s but have received more attention recently.
22chap2_p_22This User Guide outlines the following instruments:
Use of Proceeds Bonds or Loans
23chap2_p_23A use of proceeds loan or bond ties financing to specific projects and expenses (see Chapter 5: Sustainable Finance Instruments for a detailed description of use of proceeds loans and bonds).
24chap2_p_24Such instruments typically follow market best practices (e.g. relevant International Capital Market Association (ICMA) and Loan Market Association (LMA) Principles), as described in Chapter 4: Health Finance and Key Performance Indicators, as well as Chapter 5: Sustainable Finance Instruments.
Sustainability-Linked Financing (SLF): Sustainability-Linked Loans (SLL) And Sustainability-Linked Bonds (SLB)
25chap2_p_25An SLF is new funding, such as a loan or a bond, that is tied to specific Key Performance Indicators (KPIs), which are the basis for setting Sustainability Performance Targets (SPTs). The proceeds from the SLF will be allocated to the general budget.
26chap2_p_26The key component of an SLF, as opposed to a plain loan or bond (the distinction between loans and bonds is described in more detail in Chapter 5: Sustainable Finance Instruments), is that the investor is interested in the country achieving agreed performance metrics. Accordingly, the level of interest payments on the instrument will increase or decrease depending on whether the SPTs are met. For example, the SLF may outline a Human Immunodeficiency Virus (HIV) prevention performance target to be achieved within 5 years. Regular monitoring will be necessary for the performance metrics, and the country may be incentivised or penalised for over- or underachieving against these targets.
27chap2_p_27Such instruments are structured in accordance with market best practices (e.g. relevant ICMA and LMA Principles), as described in Chapter 5: Sustainable Finance Instruments.
Impact Bonds
28chap2_p_28An impact bond is a results-based financing arrangement between a government or grant funder, an investor and a service provider. The investor provides upfront funding for service delivery, and the funder only pays if pre-agreed health outcomes are achieved. Although named as a “bond”, it is not a tradable instrument; rather, it is a private investment where returns depend entirely on whether the agreed-upon outcomes are met. Impact bonds are typically small in size, usually under USD 10 million.
Debt Swaps
29chap2_p_29A debt swap is when part of a country’s debt is cancelled or replaced with cheaper debt, and the government agrees to use some, or all, of the money it saves to fund specific priority programmes. In effect, the transaction creates fiscal savings that are allocated to health expenditures. Debt swaps enable governments to earmark regular, predictable government spending over a long period, and are well-suited for funding long-term health priorities.
30chap2_p_30Two forms of debt swaps are covered in this User Guide:
- chap2_ol_1
- chap2_li_3Bilateral debt swaps. A bilateral debt swap is an agreement between a debtor country and a creditor government to cancel or convert part of the debt owed in exchange for the debtor investing an equivalent amount in agreed national projects or programmes.
- chap2_li_4Commercial debt conversions. This occurs when private sector debt is replaced with a new instrument (e.g. a new loan) under more favourable terms. Some or all of the money saved through the lower interest rate (obtained through the involvement of a credit support provider) and potentially a debt reduction is then contractually obligated to be utilised on specific spending or outcomes.
Public-Private Partnerships
31chap2_p_31A PPP is a mechanism that mobilises private funding for delivering public infrastructure and/or services. Blending commercial funding with government grants and/or concessional loans helps improve the financial viability of PPPs where projects are economically or socially essential but not commercially attractive enough for private investors.
32chap2_p_32Financing may come entirely from public sources, such as national programmes to control infectious diseases, from private sources, such as out-of-pocket expenditure for elective procedures or dentistry and from a mix of both, such as public insurance that pays for services delivered by private providers.
|
33chap2_p_33Instrument |
34chap2_p_34Primary Objective |
35chap2_p_35Typical Scale |
36chap2_p_36Relevance to Health |
37chap2_p_37Chapter |
|
38chap2_p_38Health Bonds & Loans |
39chap2_p_39The borrowed amount has to be spent on equivalent health-related expenditures |
40chap2_p_40Medium - Large |
41chap2_p_41Incentivise the increase in the health budget |
42chap2_p_42Chapter 4: Health Finance and Key Performance Indicators |
|
43chap2_p_43SLFs |
44chap2_p_44Tie borrowing costs to measurable health outcomes |
45chap2_p_45Medium - Large |
46chap2_p_46Incentivise performance and accountability |
47chap2_p_47Chapter 4: Health Finance and Key Performance Indicators |
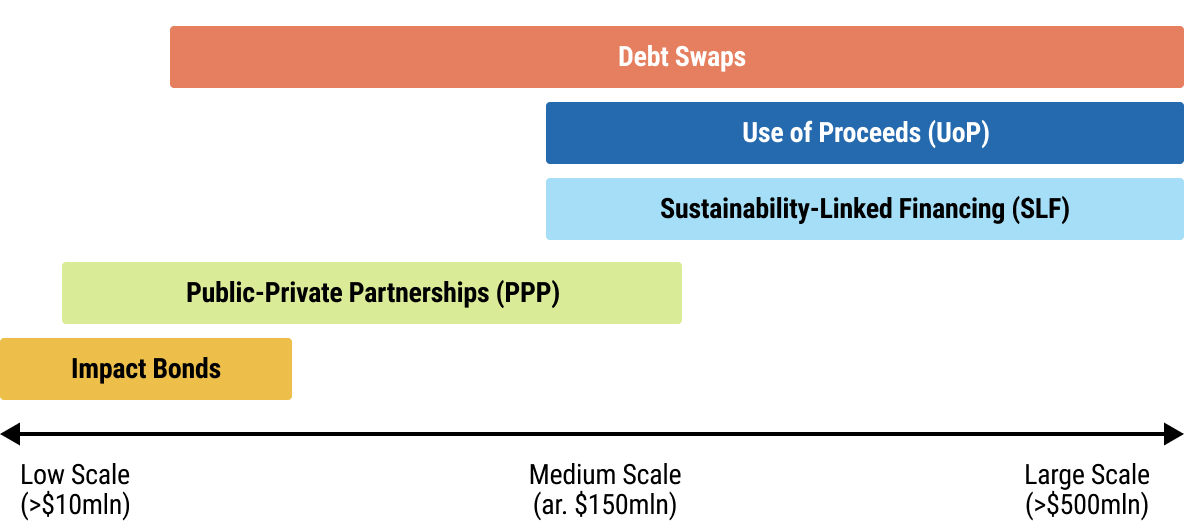
|
48chap2_p_48Impact Bonds |
49chap2_p_49Combine public and private funds to achieve pre-agreed outcome targets delivered by a service provider |
50chap2_p_50Small |
51chap2_p_51Incentivise the performance of a non-governmental implementer |
52chap2_p_52Chapter 4: Health Finance and Key Performance Indicators |
|
53chap2_p_53Debt Swaps |
54chap2_p_54Convert significant amounts of debt repayments into health investments |
55chap2_p_55Small - Medium |
56chap2_p_56Free up fiscal space for priority programmes |
57chap2_p_57Chapter 6: Debt-for-Health Swaps |
|
58chap2_p_58PPPs |
59chap2_p_59Mobilise private investment in health infrastructure/services |
60chap2_p_60Large |
61chap2_p_61Expand capacity sustainably |
62chap2_p_62Chapter 7: The Use of Public-Private Partnerships in Healthcare Projects |
Key Considerations in Selecting Instruments and Health Priorities
63chap2_p_63There are three common considerations when selecting the type of instrument to use:
Scale of Funding
64chap2_p_64Both MoHs and MoFs are interested in how much funding can be mobilised to support health or the general budget. When considering the instruments, how much money is mobilised will be a key consideration.
 chap2_img_3
chap2_img_3
Fig. 2.4: Financing Instruments
Indebtedness
65chap2_p_65In addition to considering the amount of debt raised, MoFs need to consider the country’s debt-carrying capacity (I.e. the maximum level of debt a country can sustainably incur and service without entering into financial distress). When debt levels are low, instruments such as health bonds and SLFs may be suitable as they allow governments to raise capital for sustainable development. For countries with high but still manageable debt, PPPs can be appropriate, as they mobilise private and/or concessional capital without significantly adding to public debt burdens. Note that SLFs can also help improve debt sustainability by refinancing or buying back outstanding debt.
66chap2_p_66Debt swaps can be helpful by way of liquidity support, as they offer a tailored and effective way to lower debt servicing costs and in some instances also the debt to GDP ratio of the country (especially where any publicly traded bonds repurchased as part of the debt conversion are trading at high discounts) and channel fiscal savings into health-related programmes which would otherwise be unfunded.
 chap2_img_4
chap2_img_4
Specificity
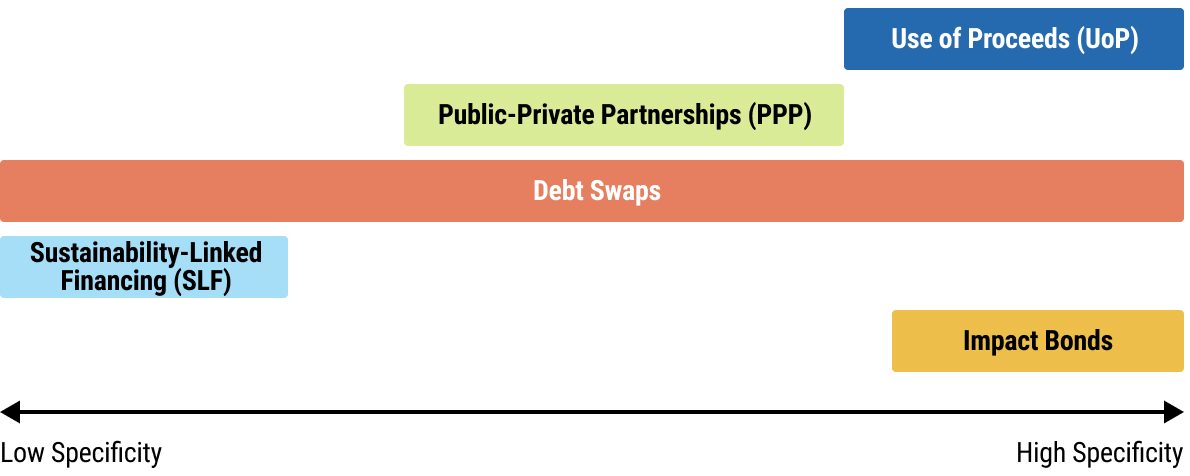
67chap2_p_67Financing instruments differ in the extent to which the funds raised must be used for specific purposes. In some cases, such as health loans, bonds and impact bonds, the funding is tied to specific activities or outcomes. Other instruments, such as SLLs and SLBs, are included in the general budget, allowing for significant flexibility in spending decisions during the implementation phase.
 chap2_img_5
chap2_img_5
